Four Reasons to Refer Your Patient to an Orthopedic Surgeon
Would you know why and/or when should you refer your patient to an orthopedic surgeon?
The answer could be somewhat tricky, especially when you have been their primary care provider for years and a non-specialist providing symptomatic management of your patient’s knee osteoarthritis. Inevitably, all patients with knee arthritis will progress to end-stage arthritis as they age. However, knowing when to refer patients out to orthopedic surgical counseling and evaluation for possible knee replacement will be easier if you keep the following four conditional circumstances in mind since this ailment/disease symptomatic time interval advances differently in most people.
1. Worsening OA symptoms:
The patient will report that their Knee pain (arthralgia), stiffness, duration, intensity, and frequency have worsened over a period of days, weeks, months, or even years since you first began managing their symptoms. They are recurring more intensely and unabating despite prior and current symptomatic treatment modalities used including PT. They even have developed nonactivity-related pain, either pain at rest or nocturnally— oftentimes both. In other words, they have pain around the clock severely impacting their lives.
2. Worsening functional abilities:
The patient will describe their activities of daily living (ADLs) have or are becoming more difficult to perform or restrictive. They have more difficulty ambulating longer distances(shopping), dressing themselves, or simply performing any household chores as they used to. Again, their Knee pain (arthralgia) has become unbearable and is the main limiting factor, thus restricting their ability to even enjoy any recreational activities they used to (i.e. bike riding, golfing, and other low-impact activities).
3. Failed Pharmacologic Pain Control:
The patient will discuss that despite the various pain medication regimen combinations tried and revised during their care, they subjectively ascribe their pain remaining most unrelieved in their view. In many cases, even injectable therapy (i.e. corticosteroids, or even Intra-articular Hyaluronic acid: Euflexa/Synvysc/Surpartz–current brand names in the marketplace) falls short of their expectations. For example, they relate the efficacy and
duration of steroid symptomatic relief have decreased considerably in their estimation compared to when initially started; instead of lasting 2 or 3 months, now it only lasts a week or 1 day in their advanced arthritic knees for which some patients would decline further continuation of this treatment modality at that point.
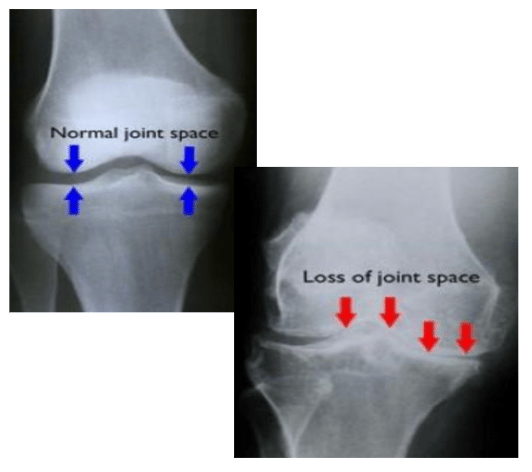
4. Worsening Radiographic Changes:
As your patient’s knee arthritis worsens symptomatically so do their radiographic findings. As time progresses, your initial and subsequent surveillance knee x-rays unequivocally confirm the initial subtle bony changes of joint-space narrowing have become bone-on-bone. Plus, now you would see the bony spurs (osteophytes) formation increase in numbers along with sclerosing lines. Also, the loss of smooth cortical bony surfaces or even the development of bony cysts would become more notable compared to when initially seen in some cases depending on the stage you assumed care of the patient during their arthritic journey.
Take Away
In the world of inter-related medicine (primary care and specialty care), collaborative practices not only plays a crucial role in providing effective comprehensive care but, more importantly, facilitate the timely adjustments to the treatment plan and patient’s emerging treatment and/or lifestyle concerns related to the burden diseased state they face.
By knowing time-specific specialty criteria referral (as discussed), the primary care provider will stand to gain optimal medical care outcomes when recognizing and addressing the needs of his patients deserving of higher care (orthopedic surgery) when clinically warranted.


